What is Mucormycosis? While people trying their best to protect themselves from COVID-19, there is another threat being posed by a fungus, which we must know and act upon. Mucormycosis, a fungal infection, is being reported in a few COVID-19 patients post-recovery.

What causes Mucormycosis?
Mucormycosis or black fungus is a complication caused by a fungal infection. People catch it by coming in contact with the fungal spores in the environment. It can also develop on the skin after the fungus enters the skin through a cut, scrape, burn, or another type of skin trauma.
Also Read | Coronavirus India: PM Narendra Modi a ‘super-spreader’ of COVID-19, says IMA Vice President

The disease is being detected among patients who are recovering or have recovered from COVID-19.
The following conditions in COVID-19 patients increase the risk of mucormycosis infection:
- Uncontrolled diabetes
- Weakening of immune system due to use of steroids
- Prolonged ICU/hospital stay
- Co-morbidities / post organ transplant / cancer
- Voriconazole therapy (used to treat serious fungal infections)
How Mucormycosis is related to COVID-19?
It is caused by a set of micro-organisms known as mucormycetes, which are present naturally in the environment, seen mostly in soil and in decaying organic matter like leaves, compost, and piles.
Also Read | Coronavirus: Delhi witnesses major decline in COVID-19 cases in 24 hours
The body’s immune system successfully fights such fungal infections, however, we know that COVID-19 affects the immune system. Moreover, the treatment of COVID-19 patients involves consuming drugs like dexamethasone, which suppresses the immune system response.
Due to these factors, COVID-19 patients face a renewed risk of failing the battle against attacks mounted by organisms such as mucormycetes.
Also, COVID patients undergoing oxygen therapy in ICU, where a humidifier is used, are prone to fungal infection because of exposure to moisture.
What are the common symptoms of Mucormycosis?
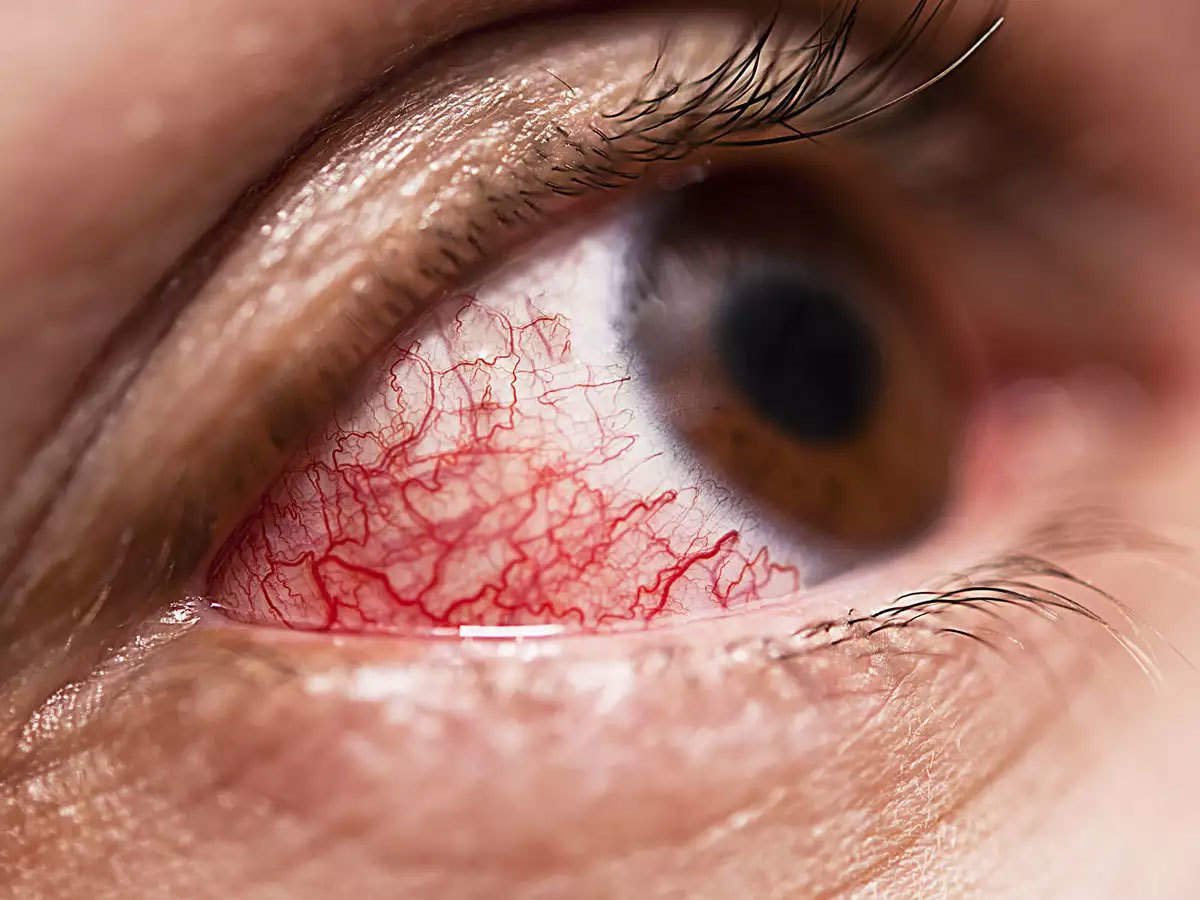
It begins to manifest as skin infection in the air pockets located behind our forehead, nose, cheekbones, and in between the eyes and teeth. It then spreads to the eyes, lungs and can even spread to the brain. It leads to blackening or discoloration over the nose, blurred or double vision, chest pain, breathing difficulties and coughing of blood.

How is it treated?
Treatment involves surgically removing all dead and infected tissue and may also involve a 4-6 weeks course of intravenous anti-fungal therapy. The treatment requires a team of microbiologists, internal medicine specialists, intensivist neurologists, ENT specialists, ophthalmologists, dentists, surgeons, and others.
Controlling diabetes is one of the foremost prevention methods suggested by ICMR. Hence, COVID-19 patients who are diabetic need to take utmost care.
Self-medication and over-dosage of steroids can result in fatal events and hence doctor’s prescription should be strictly followed.
Click here to follow PTC News on Twitter
-PTC News

 The disease is being detected among patients who are recovering or have recovered from COVID-19.
The following conditions in COVID-19 patients increase the risk of mucormycosis infection:
- Uncontrolled diabetes
- Weakening of immune system due to use of steroids
- Prolonged ICU/hospital stay
- Co-morbidities / post organ transplant / cancer
- Voriconazole therapy (used to treat serious fungal infections)
The disease is being detected among patients who are recovering or have recovered from COVID-19.
The following conditions in COVID-19 patients increase the risk of mucormycosis infection:
- Uncontrolled diabetes
- Weakening of immune system due to use of steroids
- Prolonged ICU/hospital stay
- Co-morbidities / post organ transplant / cancer
- Voriconazole therapy (used to treat serious fungal infections)
 The body’s immune system successfully fights such fungal infections, however, we know that COVID-19 affects the immune system. Moreover, the treatment of COVID-19 patients involves consuming drugs like dexamethasone, which suppresses the immune system response.
Due to these factors, COVID-19 patients face a renewed risk of failing the battle against attacks mounted by organisms such as mucormycetes.
Also, COVID patients undergoing oxygen therapy in ICU, where a humidifier is used, are prone to fungal infection because of exposure to moisture.
The body’s immune system successfully fights such fungal infections, however, we know that COVID-19 affects the immune system. Moreover, the treatment of COVID-19 patients involves consuming drugs like dexamethasone, which suppresses the immune system response.
Due to these factors, COVID-19 patients face a renewed risk of failing the battle against attacks mounted by organisms such as mucormycetes.
Also, COVID patients undergoing oxygen therapy in ICU, where a humidifier is used, are prone to fungal infection because of exposure to moisture.

